Topics
Reproduction in Lower and Higher Plants
- Reproduction
- Mode of Reproduction in Plant
- Asexual Reproduction in Plant
- Vegetative Reproduction
- Natural Vegetative Reproduction
- Artificial Vegetative Reproduction
- Sexual Reproduction in Flowering Plants
- Pre-fertilization in Plant: Structure and Events
- Pre-fertilization in Plant: Stamen (Male Reproductive Unit)
- Pre-fertilization in Plant: Microsporangium
- Structure of Microspore Or Pollen Grain
- Pre-fertilization in Plant: Pistil (Female Reproductive Unit)
- Pre-fertilization in Plant: Megasporangium
- Pre-fertilization in Plant: Formation of Embryo Sac
- Pollination
- Self Pollination (Autogamy)
- Cross Pollination
- Agents of Pollination
- Outbreeding Devices
- Pollen Pistil Interaction
- Fertilization Process
- Post Fertilisation in Plant: Structures and Events
- Development of Endosperm
- Post Fertilization in Plant: Development of Embryo (Embryogeny)
- Formation of Seed and Fruit
- Apomixis
- Parthenocarpy
- Polyembryony
- Kinds of Pollination
Reproduction in Lower and Higher Animals
- Reproduction
- Mode of Reproduction in Animal
- Asexual Reproduction in Animal
- Sexual Reproduction in Animals
- Human Reproduction
- The Male Reproductive System
- The Female Reproductive System
- Menstrual Cycle (Ovarian Cycle)
- Gametogenesis
- Fertilization in Human
- Embryonic Development in Human
- Implantation in Human
- Pregnancy in Humans
- Placenta (Growth) in Human
- Parturition (Birth) in Human
- Lactation in Human
- Reproductive Health
- Population Stabilisation and Birth Control
- Medical Termination of Pregnancy (MTP)
- Sexually Transmitted Diseases (STD)
- Infertility
- Gastrulation in humans
Inheritance and Variation
- Heredity or Inheritance
- Gregor Johann Mendel – Father of Genetics
- Genes and Genetic
- Mendelian Inheritance - Mendel’s Law of Heredity
- Back Cross and Test Cross
- Deviations from Mendel’s Findings
- Chromosomal Theory of Inheritance
- Chromosomes - The Carriers of Heredity
- Linkage and Crossing Over
- Autosomal Inheritance
- Sex Linked Inheritance
- Sex Determination
- Genetic Disorders
Molecular Basis of Inheritance
- Deoxyribonucleic Acid (DNA) and Its Structure
- The Genetic Material is a DNA
- Packaging of DNA Helix
- DNA Replication
- Protein Synthesis
- Regulation of Gene Expression
- Operon Concept
- Genomics
- Human Genome Project
- DNA Fingerprinting Technique
- Genetic Code
Origin and Evolution of Life
- Origin and Evolution of Universe and Earth
- Theories of Origin of Life
- Chemical Evolution of Life (Self-assembly Theory of the Origin of Life)
- Darwinism
- Mutation Theory
- Modern Synthetic Theory of Evolution
- Organic Evolution
- Hardy Weinberg’s Principle
- Adaptive Radiation
- Evidences for Biological Evolution
- Speciation
- Geological Time Scale
- Human Evolution
- Theories of Biological Evolution
Plant Water Relation
- Plant Water Relation
- Properties of Water
- Water absorbing organ
- Water Available to Roots for Absorption
- Means of Transport in Plants
- Concept of Imbibition
- Simple Diffusion
- Concept of Osmosis
- Osmotic Pressure
- Facilitated Diffusion
- Turgidity and Flaccidity (Plasmolysis)
- Active Transport
- Passive Transport
- Water Potential (ψ)
- Path of Water Across the Root
- Translocation of Water (Ascent of Sap)
- Transport of Mineral Ions
- Transport of Food
- Transpiration
- Types of Transpiration
- Structure of Stomatal Apparatus
- Significance of Transpiration
Plant Growth and Mineral Nutrition
- Plant Growth
- Phases of Plant Growth
- Conditions Necessary for Plant Growth
- Plant Growth Rate
- Plant Growth Curve
- Differentiation, De-differentiation, Re- Differentiation
- Plant Development
- Plant Plasticity
- Plant Hormones
- Types of Plant Hormones: Auxins
- Types of Plant Hormones: Gibberellins
- Types of Plant Hormones: Cytokinins
- Types of Plant Hormones: Ethylene
- Types of Plant Hormones: Abscisic Acid (ABA)
- Photoperiodism
- Vernalization (Yarovization)
- Plant Mineral Nutrition
- Nitrogen Cycle
Respiration and Circulation
- Respiration
- Organs of Respiratory Exchange
- Human Respiratory System
- Mechanism of respiration-Breathing
- Regulation of Breathing / Respiration
- Modified Respiratory Movements
- Disorders of Respiratory System
- Transportation in Living Organisms
- Circulation in Animals
- Types of Closed Circulation
- Blood Circulatory System in Human
- Composition of Blood: Plasma (The Liquid Portion of Blood)
- Composition of Blood: Red Blood Cells (Erythrocytes)
- Composition of Blood: White Blood Cells (Leukocytes)
- Composition of Blood: Blood Platelets (Thrombocytes)
- Function of Platelets - Clotting of Blood (Coagulation)
- Human Heart
- Working mechanism of human heart
- Blood Vessels
- Blood Pressure (B.P.)
- Electrocardiogram (ECG)
- Lymph and Lymphatic System
- Mechanism of respiration - Internal respiration
- Mechanism of respiration - External respiration
- Mechanism of respiration - Cellular respiration
Control and Co-ordination
- Control and Co-ordination
- Nervous System in Hydra
- Nervous System in Planaria (Flatworm)
- Neural Tissue
- Neuron (Or Nerve Cell) and Its Types
- Neuroglial Cells (Or Glial Cells)
- Human Nervous System
- Central Nervous System (CNS)
- The Human Brain - Forebrain
- The Spinal Cord
- Peripheral Nervous System (PNS)
- Sensory Receptors
- Human Eye
- Human Ear
- Disorders of Nervous System
- Chemical Coordination
- Human Endocrine System
- The Hypothalamus
- Pituitary Gland or Hypophysis Gland
- The Pineal Gland
- Thyroid Gland
- Parathyroid Gland
- Thymus Gland
- Adrenal Gland (Suprarenal Gland)
- Pancreas (Islets of Langerhans)
- Reproductive Glands (Gonads)
- Synapse - Properties of nerve fibres
- Synapse - Types of synapse
- Transmission of nerve impulse
- Generation of nerve impulse
- Reflex Action
- Autonomic Nervous System (ANS)
- Diffuse Endocrine Glands
Human Health and Diseases
- Defence System in Our Body: Immune System
- Immunity
- Types of Immunity
- Vaccination and Immunization
- Structure of Antibody
- Disease
- Protozoan Diseases
- Helminthic Diseases
- Bacterial Diseases
- Viral Diseases
- Fungal Diseases
- Vector Borne Diseases
- Cancer
- Adolescence
- Addiction
- Drug Abuse
Enhancement of Food Production
- Improvement in Food Production
- Plant Breeding
- Tissue Culture
- Single Cell Protein (SCP)
- Biofortification
- Animal Husbandry (Livestock)
- Animal Breeding
- Dairy Farming
- Poultry Farming
- Apiculture (Bee Farming)
- Pisciculture (Fish Farming)
- Sericulture
- Lac Culture
- Microbes in Human Welfare
- Microbes in Industrial Production
- Microbes in Sewage Treatment
- Microbes in Energy Generation
- Microbes as Biocontrol Agents
- Microbes as Biofertilizers
Biotechnology
- Biotechnology
- Process and Principles of Biotechnology
- Methodology for rDNA Technology
- Commercial Applications of Biotechnology
- Bioethics
- Effects of Biotechnology on the Environment
- Biopatent and Biopiracy
- Transgenic Plants
- Transgenic animals
- Effects of Biotechnology on Human Health
- Tools and techniques for gene cloning/ rDNA technology
Organisms and Populations
- Organisms and the Environment Around
- Habitat
- Niche
- Structure and Function of an Ecosystem
- Adaptations and Its Types
- Population
- Population Interactions
- Organisms and Populations
Ecosystems and Energy Flow
- Ecosystem
- Structure and Function of an Ecosystem
- Concept of Energy Flow in an Ecosystem
- Classification of Animal
- Trophic Level
- Food Chain
- Food Web
- Ecological Pyramids
- Nutrient Cycles
- Ecological Succession
- Ecosystem Services
- Productivity
- Decomposition
- Phosphorus Cycle
- Carbon Cycle
Biodiversity, Conservation and Environmental Issues
- Biodiversity
- Levels of Biodiversity
- Patterns of Biodiversity
- Biodiversity Current Scenario
- Loss of Biodiversity
- Conservation of Wildlife
- Biological Diversity Act, 2002
- Environmental Issues
- Air Pollution and Its Causes
- Noise Pollution
- Water Pollution and Its Causes
- Green House Effect
- Preventive Measures of Green House Effect
- Global Warming
- Preventive Measures of Global Warming
- Ozone Layer Depletion
- Deforestation and Its Causes
- Mission Harit Maharashtra
- Conservation of Biodiversity
Excretion and Osmoregulation
- Modes of Excretion: Ammonotelism, Ureotelism, and Uricotelism
- Human Excretory System
- Function of the Kidney - “Production of Urine”
- Regulation of Kidney Function
- Common Disorders of the Urinary System
Human Reproduction
- Female Reproductive System
- Ovaries
- Accessory ducts
- External genitalia
- Accessory glands
- Mammary glands
- Puberty / Sexual maturity in Females
Notes
The female reproductive system:
- The female reproductive system is far more complex than the male because, in addition to gamete formation, it has to nurture the developing foetus.
- The human female reproductive system located in the pelvic region.

Female pelvis showing reproductive system
- The female reproductive system includes:
- A pair of ovaries
- A pair of oviduct.
- Accessory ducts (Fallopian tubes, Uterus, Vagina)
- Cervix
- External genitalia (mons pubis, labia majora, labia minora, hymen, and clitoris)
- Accessory glands (Bartholin's glands, Skene's tubules)
- A pair of mammary gland

Diagrammatic view of female reproductive system
- These parts along with the mammary glands are integrated structurally and functionally to support the process of ovulation, Fertilization, pregnancy, child birth, and child care.
A) Ovaries:
- It is the primary female sex organ. Its main function is production of egg or ovum and the female reproductive hormones.
- It is a solid, oval or almond shaped organ. It is 3.0 cm in length, 1.5 cm in breadth and 1.0 cm thick. It is in the upper lateral part of the pelvis near the kidneys.
- Each ovary is covered by a thin cuboidal epithelium called the germinal epithelium which encloses the ovarian stroma.
- The ovarian stroma has two zones - A peripheral cortex and an inner medulla.
- Below the germinal epithelium is a dense connective tissue, the tunica albuginea.
- The cortex appears dense and granular due to the presence of ovarian follicles in various stages of development.
- The medulla is a loose connective tissue with abundant blood vessels, lymphatic vessels, and nerve fibres.
- The ovary remains attached to the pelvic wall and the uterus by an ovarian ligament called mesovarium.
Structure and development of the ovary:
- Each ovary is a compact structure differentiated into a central part called medulla and the outer part called cortex.
- The outer cortex is more compact and granular. It shows large number of tiny masses of cells called ovarian follicles.
- These are collectively formed from the immature ova originating from cells of the dorsal endoderm of the yolk sac. The cells migrate to the gonadal ridge during embryonic development and divide mitotically. Now these cells are called oogonia.
- The process of oogenesis starts much before the birth of the female baby and by the end of twelve weeks the ovary is fully formed. It has more than two million primordial follicles in it.
- Each primordial follicle has, at its center a large primary oocyte (2n) surrounded by a single layer of flat follicular cells.
- The development of the primordial follicles into mature or Graafian follicles restarts with the onset of puberty. During each menstrual cycle only one of the primordial follicle starts growing to form the Graafian follicle.
- The stage of follicles develops alternately in the ovary throughout the menstrual cycle, influenced by pituitary and ovarian hormones.
- The 1st menstrual cycle or menarche begins normally at about 13 years and Menopause i.e. stopping of the cycles happens at age 45 to 55 years.
- The reproductive age of the female and is approximately 32 years. In this time the female will be producing a maximum of about 416 eggs (32 ×13 = 416 eggs).
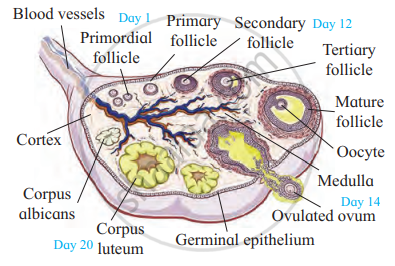
T.S. of ovary
Ovarian histology of a mature female-
- Changes in the ovary are cyclic, occurring during each menstrual cycle and it involves maturation of the primordial follicles into primary, secondary and Graafian follicles.
- Each primary follicle has multilayered cuboidal follicular cells. The stroma cells add theca over the follicle. It now changes into a secondary follicle.
- The egg is released from the Graafian follicle during ovulation and the remaining part of the follicle changes into a temporary endocrine gland called corpus luteum. If fertilization does not take place the corpus luteum degenerates into a white scar called corpus albicans.
Structure of Graafian follicle-
- Graafian follicle is a mature ovarian follicle. An eccentric secondary oocyte is surrounded by a non-cellular layer of zona pellucida secreted by the vitelline membrane of oocyte. The outermost protective and fibrous covering is called theca externa. Inner to it is cellular theca interna.
- It produces the hormone estrogen. Inner to the theca interna, the follicular cells form the membrana granulosa. From the membrana granulosa the cells differentiate into discus proligerus and the corona radiata cells.
- A fluid filled cavity called antrum lies between the oocyte and the membrana granulosa. It is filled with a fluid called liquor folliculi.
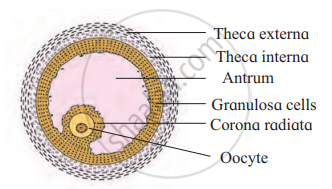
Graafian Follicle
B) Accessory ducts:
The fallopian tubes (uterine tubes or oviducts), uterus, and vagina constitute the female accessory organs.
1) Oviduct (fallopian tube):
- Each fallopian tube extends from the periphery of each ovary to the uterus.
- Each oviduct (10-12 cm long) has 3 parts:
i) Infundibulum: The proximal part of the fallopian tube bears a funnel-shaped infundibulum. The edges of the infundibulum have many finger like projections called fimbriae which help in collection of the ovum after ovulation.
ii) Ampulla: The infundibulum leads to a wider central portion called the ampulla.
iii) Isthmus: The last part of the oviduct is the isthmus which is short and thick-walled connecting the ampulla and infundibulum to the uterus.
2) Uterus:
- The uterus or womb is a hollow, thick-walled, muscular, highly vascular, and inverted pear-shaped structure lying in the pelvic cavity between the urinary bladder and rectum.
- The major portion of the uterus is the body and the rounded region superior to it, is the fundus.
- The uterus opens into the vagina through a narrow cervix. The cavity of the cervix called the cervical canal communicates with the vagina through the external orifice and with the uterus through the internal orifice.
- The cervical canal along with the vagina forms the birth canal.
- The wall of the uterus has three layers of tissues.
i) Perimetrium: The outermost thin membranous serous layer called the perimetrium.
ii) Myometrium: The middle thick muscular layer called the myometrium. The myometrium exhibits strong contraction during delivery of the baby in response to oxytocin.
iii) Endometrium: The inner glandular layer called endometrium. The endometrium undergoes cyclic changes during the menstrual cycle.
3) Vagina:
- Vagina is a large fibromuscular tube that extends from the cervix to the exterior. It is the female organ of copulation.
C) External genitalia (or vagina or vulva):
The female external genitalia includes the mons pubis, labia majora, labia minora, hymen, and clitoris.
- Mons pubis: Mons pubis is a cushion of fatty tissue covered by skin and pubic hair.
- Labia majora: The labia majora are fleshy folds of tissue, which extend down from the mons pubis and surround the vaginal opening.
- Labia minora: The labia minora are paired folds of tissue under the labia majora.
- Hymen: The opening of the vagina is often covered partially by a membrane called hymen. The hymen is often torn during the first coitus (physical union). However, in some women, it remains intact. It can be stretched or torn due to a sudden fall or jolt and also during strenuous physical activities such as cycling, horseback riding, etc., and therefore cannot be considered as an indicator of a woman’s virginity.
- Clitoris: The clitoris is a tiny finger-like structure which lies at the upper junction of the two labia minora above the urethral opening.
D) Accessory glands:
- Bartholin's glands: The Bartholin’s glands (also called greater vestibular glands) are located posterior to the left and right of the opening of the vagina. They secrete mucus to lubricate the vagina and are homologous to the bulbourethral glands of the male.
- Skene’s glands: The Skene’s glands are located on the anterior wall of the vagina and around the lower end of the urethra. They secrete a lubricating fluid and are homologous to the prostate gland of males.
E) Mammary gland:
- The mammary glands are modified sweat glands present in both sexes.
- It is rudimentary in the males and functional in the females.
- A pair of mammary glands is located in the thoracic region.
- It contains glandular tissue and variable quantities of fat with a median nipple surrounded by a pigmented area called the areola.
- Several sebaceous glands called the areolar glands are found on the surface and they reduce cracking of the skin of the nipple.
- Internally each mammary gland consists of 2-25 lobes, separated by fat and connective tissues.
- Each lobe is made up of lobules which contain acini or alveoli lined by epithelial cells.
- Cells of the alveoli secrete milk.
- The alveoli open into mammary tubules. The tubules of each lobe join to form a mammary duct. Several mammary ducts join to form a wider mammary ampulla which is connected to the lactiferous duct in the nipple.
- Under the nipple, each lactiferous duct expands to form the lactiferous sinus which serves as a reservoir of milk.
- Each lactiferous duct opens separately by a minute pore on the surface of the nipple.
- Normal development of the breast begins at puberty and progresses with changes during each menstrual cycle.
- In non-pregnant women, the glandular structure is largely underdeveloped and the breast size is largely due to amount of fat deposits. The size of the breast does not have an influence on the efficiency of lactation.
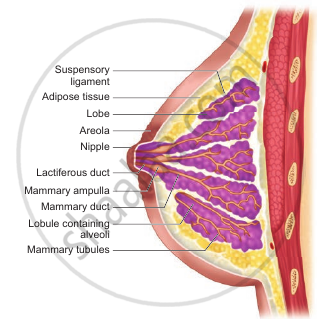
Mammary glands
Puberty / Sexual maturity in Females:
- The reproductive system becomes functional at puberty. It is characterized by onset of menstrual cycle also called menarche, which usually occurs at age 10- 14 years.
- Menstrual cycle continues only upto menopause. Both are controlled by gonadotropic hormones.
If you would like to contribute notes or other learning material, please submit them using the button below.
Shaalaa.com | Female Reproductive System: Fallopian tube
to track your progress
Series: series 1
0%
